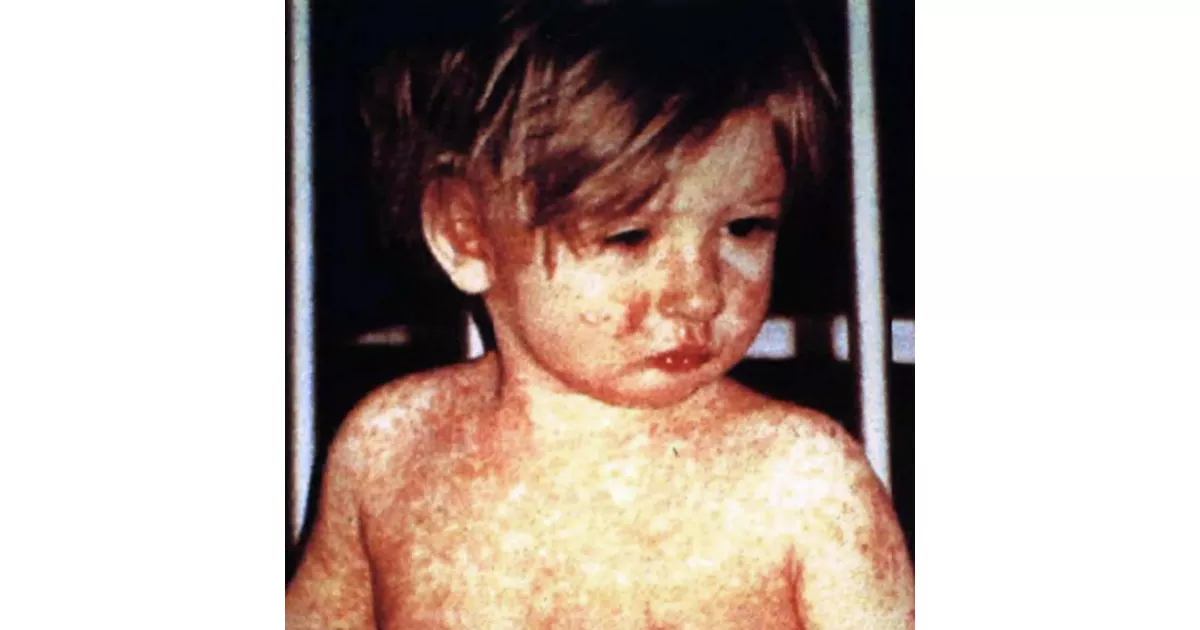
Measles, also known as morbilli, rubeola, 9-day measles, red measles, or English measles, is a highly contagious infectious disease caused by the measles virus. It is vaccine-preventable, making immunization the primary means of control and eradication. Due to its contagiousness, measles can spread rapidly among unvaccinated populations. Symptoms typically include fever, cough, runny nose, and a characteristic skin rash. Complications can be severe, especially in young children and immunocompromised individuals. Vaccination efforts have dramatically reduced the global incidence of measles, highlighting the importance of herd immunity.
1914: Measles Mortality Estimate
In 1914, a statistician for the Prudential Insurance Company estimated that 1% of all deaths in the temperate zone were caused by measles. He also observed that 1–6% of cases of measles ended fatally, with the difference depending on age, social conditions, and pre-existing health conditions.
1954: Isolation of Measles Virus
In 1954, John Enders and Thomas C. Peebles isolated the measles virus from a 13-year-old boy from the United States, David Edmonston. Enders used similar techniques to grow the Edmonston strain in human kidney tissue, amniotic membrane tissue culture, and chick embryo culture.
1957: Presumptive evidence of measles immunity
Birth before 1957 is presumptive evidence of immunity because people born before 1957 are likely to have been naturally infected with the measles virus.
1957: Critical Community Size Concept
In 1957, M.S. Bartlett recognized the concept of the critical community size (CCS) for measles, referring to the minimum number of people required to sustain the disease.
1963: Atypical measles vaccine use
Between 1963 and 1967, the inactivated measles vaccine was used and caused atypical measles.
1963: First Successful Measles Vaccine
In 1963, the first successful measles vaccine was developed by Maurice Hilleman at Merck, becoming widely available in the United States. This vaccine was associated with post-immunization reactions including fever and rash.
1965: Introduction of Schwartz Strain Measles Vaccine
In 1965, the Schwartz strain was introduced to reduce reactions from the measles vaccine. It is no longer used.
1967: Discontinuation of Killed Measles Vaccine
Between 1963 and 1967 a killed measles vaccine was given, but it was discontinued in favor of the live-attenuated vaccine due to the risk of atypical measles and inferior protection.
1967: Atypical measles vaccine use
Between 1963 and 1967, the inactivated measles vaccine was used and caused atypical measles.
1968: Introduction of Edmonston-Enders Strain
In 1968, the Edmonston-Enders strain of the measles vaccine was introduced to reduce reactions.
1971: Licensing of MMR Vaccine
In 1971, the measles vaccine was combined with the mumps vaccine and rubella vaccine to create the MMR vaccine, which was then licensed for use in the United States.
1975: Discontinuation of Edmonston B
In 1975, Edmonston B measles vaccine was discontinued.
1980: Measles deaths
In 1980, 2.6 million people died from measles.
1985: Measles death rate in the U.S.
Between 1985 and 1992, the death rate for measles cases reported in the U.S. was 0.2%.
1987: Measles fatality rate in the U.S.
Between 1987 and 2000, the case fatality rate across the United States was three deaths per 1,000 cases attributable to measles, or 0.3%.
1990: Measles deaths
In 1990, 545,000 people died from measles.
1991: Measles Outbreak in Philadelphia
In 1991, an outbreak of measles in Philadelphia centered around the Faith Tabernacle Congregation, where members were discouraged from vaccinating their children. Over 1400 people were infected, and nine children died.
1992: Measles death rate in the U.S.
Between 1985 and 1992, the death rate for measles cases reported in the U.S. was 0.2%.
1992: Measles Cases Confirmed in the U.S.
From January to December 2019, 1,282 individual cases of measles were confirmed in 31 states in the US. This was the greatest number of cases reported in the U.S. since 1992. Of the 1,282 cases, 128 people were hospitalized, and 61 reported having complications, including pneumonia and encephalitis.
1996: Global measles cases increased
By 2019, cases had increased to a total of 870,000, the highest since 1996.
1997: Significant Increase in Measles Cases in Europe
In 2024, there were 127,350 cases reported in Europe, which was the highest caseload in the region since 1997.
1999: Measles deaths
Worldwide, measles fell 60% from an estimated 873,000 deaths in 1999 to 345,000 in 2005.
2000: Measles Cases Reported in 22 States
As of April 2019, 695 cases of measles had been reported in 22 states in the US. This was the highest number of measles cases since measles was declared eliminated in 2000.
2000: Measles fatality rate in the U.S.
Between 1987 and 2000, the case fatality rate across the United States was three deaths per 1,000 cases attributable to measles, or 0.3%.
2000: Global measles cases decreased
Between 2000 and 2016, global measles cases decreased by 84%.
2000: Decrease in measles deaths due to vaccination
Between 2000 and 2017, vaccination resulted in an 80% decrease in deaths from measles.
2000: Measles Declared Eliminated in the United States
In 2000, the United States was declared free of circulating measles due to widespread vaccination efforts.
2000: Establishment of the Global Measles and Rubella Laboratory Network (GMRLN)
In 2000, the WHO established the Global Measles and Rubella Laboratory Network (GMRLN) to provide laboratory surveillance for measles, rubella, and congenital rubella syndrome.
2001: Measles Cases in the United States
From 2001 to 2011, the United States reported 911 cases of measles.
2001: Eradication of Rinderpest
In 2001, Rinderpest, a cattle virus closely related to the measles virus, was eradicated.
2003: Measles Death in Washington State
In 2015, a woman in Washington state died of pneumonia as a complication of measles, marking the first measles fatality in the U.S. since 2003. The woman had been vaccinated but was taking immunosuppressive drugs.
2005: Licensing of MMRV Vaccine
In 2005, the MMR vaccine was combined with the varicella vaccine to create the MMRV vaccine, which was then licensed.
2005: Measles deaths
Worldwide, measles fell 60% from an estimated 873,000 deaths in 1999 to 345,000 in 2005.
2007: Measles death rates in England and Wales
From 2007 to 2017, death occurred between two and three cases out of 10,000 in England and Wales.
2008: Global measles deaths
Estimates for 2008 indicate deaths fell further to 164,000 globally, with 77% of the remaining measles deaths in 2008 occurring within the Southeast Asian region.
2011: Measles Cases in the United States
From 2001 to 2011, the United States reported 911 cases of measles.
2011: Stefan Lanka's Measles Challenge
In 2011, German anti-vaccination campaigner Stefan Lanka offered €100,000 to anyone who could scientifically prove that measles is caused by a virus and determine the virus's diameter, claiming the illness is psychosomatic and the virus doesn't exist.
2011: WHO Estimate of Measles Deaths
In 2011, the WHO estimated that 158,000 deaths were caused by measles.
2012: Decrease in measles deaths
In 2012, the number of deaths due to measles was 78% lower than in 2000 due to increased rates of immunization among UN member states.
2013: Measles cases in Europe
In 2013, there were almost 10,000 cases in 30 European countries.
October 2014: Measles outbreak in Berlin
Between October 2014 and March 2015, a measles outbreak in the German capital of Berlin resulted in at least 782 cases.
December 2014: Disneyland Measles Outbreak
In late December 2014, an outbreak of measles traced back to Disneyland theme park in California resulted in 147 people being infected across seven U.S. states, Mexico, and Canada. Most of those infected were either unvaccinated or had unknown vaccination status.
2014: Measles deaths
By 2014, global vaccination programs had reduced the number of deaths from measles to 73,000.
2014: Measles Outbreak in Ohio
In 2014, a measles outbreak began in Ohio after two unvaccinated Amish men returned from missionary work in the Philippines. The outbreak led to 383 cases across nine counties, with 89% of the cases occurring in unvaccinated individuals.
2014: CDC Statement on Measles Elimination
In 2014, the CDC stated that endemic measles, rubella, and congenital rubella syndrome had not returned to the United States, while also recommending vaccinations to prevent outbreaks from imported cases.
2014: Vietnamese Measles Epidemic
In the spring of 2014, Vietnam experienced a measles epidemic with approximately 8,500 reported cases as of April 19 and 114 fatalities. By May 30, there were 21,639 suspected measles cases reported, along with 142 measles-related fatalities.
March 2015: Measles outbreak in Berlin
Between October 2014 and March 2015, a measles outbreak in the German capital of Berlin resulted in at least 782 cases.
April 2015: Measles Cases Reported to CDC
Between January 4th and April 2nd, 2015, 159 cases of measles were reported to the CDC, with 70% linked to an earlier exposure in December 2014.
2015: Measles Outbreak in Texas and New Mexico
As of February 2025, an outbreak of measles was ongoing amongst unvaccinated communities in Texas and New Mexico. On February 26th, the first measles death since 2015 was reported in West Texas.
2015: Measles Death in Washington State
In 2015, a woman in Washington state died of pneumonia as a complication of measles, marking the first measles fatality in the U.S. since 2003. The woman had been vaccinated but was taking immunosuppressive drugs.
August 2016: Measles Outbreak in Myanmar
In August 2016, at least 40 children died during a measles outbreak in the Naga Self-Administered Zone in a remote northern region of Myanmar. The outbreak was probably caused by a lack of vaccination.
2016: Global measles cases decreased
Between 2000 and 2016, global measles cases decreased by 84%.
2016: Measles virus genotypes are decreasing
Data from 2016 to 2018 show that the most frequently detected measles virus genotypes are decreasing, suggesting that increasing global population immunity has decreased the number of chains of transmission.
2016: Brazil Wins Measles Elimination Certificate
In 2016, Brazil was awarded a measles elimination certificate by the Pan American Health Organization.
2016: Cochrane review of vitamin A supplementation
In 2016, a Cochrane review of vitamin A supplementation in children with measles found no trials assessing whether vitamin A prevents blindness.
2016: Measles cases in Europe reported
In 2016, a record low of 4,400 measles cases in Europe were reported.
2016: Measles Eliminated from the Americas
In 2016, measles was declared eliminated from the Americas because of widespread vaccination efforts.
2016: Measles Interruption in Brazil
In 2016, the spread of measles had been interrupted in Brazil, with the last-known case twelve months earlier in the state of Ceará.
June 2017: Measles Case Confirmed in Maine
In June 2017, the Maine Health and Environmental Testing Laboratory confirmed a case of measles in Franklin County, marking the first case of measles in Maine in 20 years.
2017: Measles vaccination statistics
As of 2017, approximately 85% of children worldwide had received their first dose of the measles vaccine. Also, rates of disease and deaths have increased from 2017 onwards due to a decrease in vaccination.
2017: Measles death rates in England and Wales
From 2007 to 2017, death occurred between two and three cases out of 10,000 in England and Wales.
2017: Measles resurgence in Europe
From 2017, a measles resurgence in Europe started to occur with numbers increasing to 21,315 cases, with 35 deaths.
2017: Measles deaths
In 2017, 124,000 deaths were reported due to measles infection globally.
2017: Measles reproductive number estimates review
In 2017, a review of measles's reproductive number estimates gave a range of 3.7 to 203.3.
2017: Measles cases in Americas
In 2017, after having been previously eliminated, measles cases re-appeared in the Americas.
2017: Measles Outbreak in Brooklyn
In April 2019, New York Mayor Bill de Blasio declared a public health emergency due to a "huge spike" in cases of measles where there were 285 cases centered on the Orthodox Jewish areas of Brooklyn in 2018, while there were only two cases in 2017.
July 2018: Measles Case in Portland, Oregon
In July 2018, a measles case occurred in Portland, Oregon, exposing 500 people; 40 of whom lacked immunity and were monitored by health officials.
October 2018: Measles Outbreak in Brooklyn
Starting in October 2018, a measles outbreak in Brooklyn resulted in more than 200 reported cases by February 2019. The outbreak was linked to the Orthodox Jewish community, with the initial exposure from an unvaccinated child who contracted measles while visiting Israel.
2018: Measles deaths
As of 2018, measles remains a leading cause of vaccine-preventable deaths in the world.
2018: Measles virus genotypes are decreasing
Data from 2016 to 2018 show that the most frequently detected measles virus genotypes are decreasing, suggesting that increasing global population immunity has decreased the number of chains of transmission.
2018: Measles cases in Americas
In 2018, after having been previously eliminated, measles cases re-appeared in the Americas.
2018: Measles Outbreak in Brooklyn
In April 2019, New York Mayor Bill de Blasio declared a public health emergency due to a "huge spike" in cases of measles where there were 285 cases centered on the Orthodox Jewish areas of Brooklyn in 2018, while there were only two cases in 2017.
2018: Vaccination Rate in Samoa
In December 2019, a vaccination campaign in Samoa brought the measles vaccination rate from 31 to 34% in 2018 to an estimated 94% of the eligible population.
February 2019: Measles Outbreak in Brooklyn
Starting in October 2018, a measles outbreak in Brooklyn resulted in more than 200 reported cases by February 2019. The outbreak was linked to the Orthodox Jewish community, with the initial exposure from an unvaccinated child who contracted measles while visiting Israel.
April 2019: Measles Resurgence in the U.S.
In April 2019, New York Mayor Bill de Blasio declared a public health emergency due to a significant spike in measles cases, with 285 cases centered on the Orthodox Jewish areas of Brooklyn, while there were only two cases in 2017. As of April 2019, there had been 695 cases of measles reported in 22 states, marking the highest number of cases since measles was declared eliminated in 2000.
April 2019: Measles Cases Reported in 22 States
As of April 2019, 695 cases of measles had been reported in 22 states in the US. This was the highest number of measles cases since measles was declared eliminated in 2000.
May 2019: Measles Outbreak Among Malaysian Orang Asli
From May 2019, a measles outbreak occurred among the Malaysian Orang Asli sub-group of Batek people in the state of Kelantan, resulting in the deaths of 15 people from the tribe.
December 2019: Measles Cases Confirmed in the U.S.
From January to December 2019, 1,282 individual cases of measles were confirmed in 31 states in the US. This was the greatest number of cases reported in the U.S. since 1992. Of the 1,282 cases, 128 people were hospitalized, and 61 reported having complications, including pneumonia and encephalitis.
December 2019: Vaccination Campaign in Samoa
In December 2019, a vaccination campaign in Samoa brought the measles vaccination rate from 31 to 34% in 2018 to an estimated 94% of the eligible population.
2019: Global measles cases increased
By 2019, cases had increased to a total of 870,000, the highest since 1996.
2019: Measles cases in Americas
In 2019, after having been previously eliminated, measles cases re-appeared in the Americas.
2019: Measles Outbreak
In 2019, an outbreak of measles resulted in nearly 5,000 deaths and 250,000 infections, after the disease spread to all provinces in the country. The World Health Organization (WHO) has reported this as the world's largest and fastest-moving epidemic.
2020: Measles Cases in US
Following the end of the 2019 outbreak, reported cases fell to pre-outbreak levels: 13 cases in 2020.
2020: Impact of COVID-19 pandemic
In 2020, the number of reported measles cases was lower compared to 2019. According to the WHO, the COVID-19 pandemic hindered vaccination campaigns in at least 68 countries, causing increased risk of additional cases.
2021: Measles Cases in US
Following the end of the 2019 outbreak, reported cases fell to pre-outbreak levels: 49 cases in 2021.
2022: Measles Cases in US
Following the end of the 2019 outbreak, reported cases fell to pre-outbreak levels: 121 cases in 2022.
2023: Increase in Measles Cases
In November 2024, the WHO and CDC reported that measles cases increased by 20% in 2023, primarily due to insufficient vaccine coverage in the world's poorest and conflict-affected regions, increasing from about 8.6 to 10.3 million cases.
February 2024: Risk of Measles Outbreak
In February 2024, the World Health Organization said more than half of the world was at risk of a measles outbreak due to COVID-19 pandemic-related disruptions.
November 2024: Increase in Measles Cases
In November 2024, the WHO and CDC reported that measles cases increased by 20% in 2023, primarily due to insufficient vaccine coverage in the world's poorest and conflict-affected regions, increasing from about 8.6 to 10.3 million cases.
2024: Measles Cases and Deaths Recorded by CDC
As of March 2025, the CDC had recorded 483 confirmed measles cases across 20 states, along with 2 deaths and 70 hospitalizations. This exceeded the entire 2024 total of 285 cases.
2024: Significant Increase in Measles Cases in Europe
In 2024, Europe experienced a significant surge in measles cases, with 127,350 cases reported. This was the highest number of cases since 1997, constituting one-third of the global measles cases. Romania appeared to be the epicenter, with 30,692 cases reported.
2024: Measles Outbreak Declared in Bangsamoro, Philippines
In 2024, a measles outbreak was declared in the Bangsamoro region in the Philippines, with at least 592 cases and 3 deaths.
February 2025: Measles Outbreak in Texas and New Mexico
As of February 2025, an outbreak of measles was ongoing amongst unvaccinated communities in Texas and New Mexico. On February 26th, the first measles death since 2015 was reported in West Texas. The confirmed number of cases in this outbreak was 124 as of February 26th, according to the Texas Department of Health Services, mostly in children ages 5–17.
March 2025: Measles Cases and Deaths Recorded by CDC
As of March 2025, the CDC had recorded 483 confirmed measles cases across 20 states, along with 2 deaths and 70 hospitalizations. This exceeded the entire 2024 total of 285 cases.
May 2025: Measles Outbreak in West Texas
As of May 2025, during the Southwest United States measles outbreak, Robert F. Kennedy Jr., promoted vitamin A as a treatment and prevention leading to negative side effects. Kennedy has been widely criticized for these views.
August 2025: Measles Outbreak in Alberta
As of August 2025, an outbreak of measles in Alberta resulted in 1800 confirmed cases, prompting health experts to advise Albertans to ensure their measles vaccinations were up to date.
2025: Measles cases in Americas
In 2025, after having been previously eliminated, measles cases re-appeared in the Americas.
2025: Vitamin A Treatment for Measles
In the 2025 U.S. outbreak, children are presenting at hospitals with measles and hypervitaminosis A because their parents were administering vitamin A sources (supplements or cod liver oil) as attempts of protection before the children became ill with measles.
Mentioned in this timeline
Ukraine is a country in Eastern Europe the second-largest on...
Nigeria located in West Africa is the continent's most populous...
Venezuela officially the Bolivarian Republic of Venezuela is a country...
Sudan officially the Republic of the Sudan is a country...
Myanmar also known as Burma is a Southeast Asian country...

Disneyland located in Anaheim California is a theme park owned...
Trending
48 minutes ago Senator questions TikTok's US future despite spin-off deal, citing national security risks.
2 hours ago Cody Haddon discusses injuries, career uncertainty before Aoriqileng fight at UFC Macau.
3 hours ago Milwaukee Traffic Snarled by Street Closures and Construction, Causing Rush Hour Issues.

4 hours ago Kill Bill 20th Anniversary: 4K Blu-ray Release and Streaming Success

5 hours ago Emily Blunt shines in Spielberg's 'Disclosure Day': Early reactions praise performance.
5 hours ago Alex Vesia's improbable journey from Division II walk-on to Dodgers' high-leverage hero.
Popular

Ken Paxton is an American politician and lawyer serving as...

Michael Joseph Jackson the King of Pop was a highly...

William Franklin Graham III known as Franklin Graham is an...
Graham Cunningham Platner is an American oyster farmer and Marine...

E Jean Carroll is an American journalist author and advice...

Blackpink is a South Korean girl group formed by YG...